Validating a disinfectant
for a life science cleanroom
Life science cleanroom facilities must know that the disinfectants they are using can achieve effective levels of microbial kill across a range of surface types. There are many different types and formats of disinfectants now available for use within pharmaceutical cleanrooms and there are various national and international efficacy testing standards available to compare and qualify them.
The various standards and methods available to qualify disinfectant efficacy use different methodologies and have not been written specifically for cleanroom disinfectants, so the microbial test expectations are not always suitable. There are currently differences between EU and US testing methodologies.
The expectation of regulators such as the United States Environmental Protection Agency (US EPA) and the European Chemicals Agency (ECHA) who are responsible for the safety of disinfectants / biocides placed on their respective markets and the regulators responsible for the safe manufacturing of medical products such as the FDA and the MHRA all differ.
Disinfectant Qualification and Validation
The validation of a disinfectant to be used in a pharmaceutical cleanroom forms part of the facility’s contamination control strategy and will include many factors. These will include but are not limited to, wet contact time (in vitro and in use) unopened and in-use shelf life, sterility, residues, application methods, storage, disposal, health and safety, audit of manufactuer as well as the key factor of proving that the disinfectants being used can achieve the required levels of microbial kill on the key surfaces in the cleanroom.
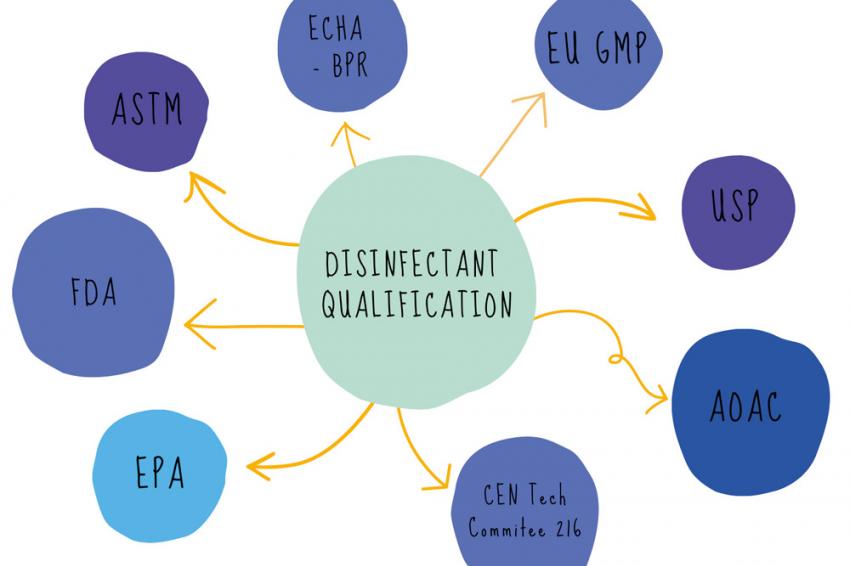
There are many acronyms that will be used when discussing disinfectants and their validation, FDA, EPA, BPR, AOAC, EN, EU GMP, USP, ASTM and the list goes on! The regulatory web can get quite confusing, especially if disinfectants are being qualified for use in different countries.
Four main groups
We can simplify the web by separating out the regulatory and testing bodies into four main groups:
- Regulatory bodies responsible for making sure biocides / disinfectants placed on their respective markets are both safe and efficacious.
- Regulatory bodies responsible for ensuring the safety of medicinal products in their respective markets.
- Organisations with approved testing methods for disinfectant efficacy qualification.
- Supporting organisations with guidance documents.
Disinfectant / biocide authorisation
In many, if not most countries, disinfectants must be authorised by the relevant regulatory authority before a manufacturer / supplier can place the product on the market. In the European Union and the UK, all biocides must be authorised for sale under the EU Biocidal Products Regulation (BPR)1 and the GB Biocidal Products Regulation (GB BPR) respectively. In the United States disinfectants, sanitizers, and sterilants are regulated by the Environmental Protection Agency (EPA) under the authority of the Federal Insecticide, Fungicide, and Rodenticide (FIFRA) Act.2
European Union
Since 1st September 2013, national biocide registrations in the EU have been replaced by one common approvals process (EU No 528/2012) the Biocidal Products Regulation. The BPR is implemented by the European Chemicals Agency (ECHA). All biocidal products require an authorisation before they can be placed on the market, and the active substances contained in that biocidal product must have been previously approved. The BPR is currently an on-going process so national registrations apply until the active substance used in a biocidal product is approved at which point a disinfectant manufacturer has 18 months to submit a dossier for authorisation in all member states they wish to sell.
It is very clear within the regulation that it is the “intent of a formulation which determines its definition as a biocide.” The absence of a claim on either literature or packaging does not mean the product is not a biocide and doesn’t need to be authorised. It costs many 1000’s euros to provide all the information required for biocidal authorisation and submit for Union (all countries) authorisation or authorisation in multiple countries. Not all cleanroom disinfectants, which include presaturated wipes have been submitted for approval due to the high costs involved. The format of the disinfectants doesn’t matter, whether it is in a trigger spray, presaturated or saturate at point-of-use wipe, a two part system which needs to be mixed, or that it is being gassed or fogged it still needs to be authorised in the manner in which it will be used.
Some examples of biocidal active ingredients commonly seen in cleanroom disinfectants are IPA and denatured ethanol hypochlorites, hydrogen peroxide, peracetic acid, quaternary ammonium compounds and phenols.
ECHA publishes a guidance docuement for suppliers “Guidance on the Biocidal Products Regulation Vol II, Efficacy” 3 which gives detailed information on what test work needs to be submitted to show a product is efficacious. This also forms a really good basis for any cleanroom facility starting disinfectant efficacy testing. It states that standard test methods and standard species should be used. Only quantitative test methods should be used, and it recommends that a tiered approach to testing is followed. Additional test organisms can be used but only if their relevance is justified and the relevant test must also be passed with standard organisms. Both the site and method of application must be specified, ie wiping in a cleanroom. The testing of the product should be appropriate for the application method, a suspension test could only be used if the surface to be disinfected was to be immersed for instance. Test methods do exist for surface testing both with and without mechanical action.
ECHA recommends that a manufacturer ideally uses internationally recognised test methods such as CEN, OECD or ISO. The use of CEN test methods is highly recommended; if no CEN test exists then OECD test methods maybe used. Other test methods are available eg AOAC, ASTM, US-EPA, VAH, AFNOR but these can only be used when there is no international standard available for a specific application.
With the introduction of disinfectant efficacy test methods from CEN Technical Committee (TC/216) a wide range of harmonised European methods for testing the activity of disinfectants used in medical, veterinary, food, industrial, domestic and institutional areas are available. TC/216 proposed a three-phase evaluation process for disinfectant efficacy testing. ECHA states that existing guidelines can be modified to make them more suitable for the specific product or conditions, for example contact time, soiling but it must be clearly described and justified. Similarly, test conditions can be modified if the claimed use of the product is different from the obligatory test conditions.
When carrying out the tesing, consideration should be given to temperature, contact time (must be practical in real life), neutralisation validation, pH, texture of surfaces, repetition of tests, pass criteria and the need for an interferring substance. In this instance, ECHA recognises that cleanrooms are a special case and that even the clean conditions of the EN test methods are overkill and WFI can be used as the interferring substance. The guidance also makes specific comment about testing disinfectant wipes, Phase 1, step 1 test should be carried out with fluid extracted from the wipe and phase 2, step 2 tests should be done with mechanical action.
United States
Under the Federal Insecticide, Fungicide, and Rodenticide (FIFRA) Act, any substance that prevents, destroys, repels, or mitigates pests, including microorganisms, is considered a pesticide 2. Chemical disinfectants are considered antimicrobial pesticides. A disinfectant manufacturer in the USA must register their product including fees with the EPA, and with every individual state they wish to sell in. A product is approved, when the EPA concludes that it is safe and effective when used as directed by the label, which includes chemical characterization, safety, and efficacy data.
Data demonstrating the efficacy claim of a disinfectant, whether it is bactericidal, fungicidal, sporicidal or viricidal, is a clear requirement of the EPA for a disinfectant manufacturer to achieve registration. Some key points expected by the EPA are that the data should be generated in compliance with Good Laboratory Practice Regulations (GLP) and that disinfectant manufacturers, test products for biocidal efficacy at the active ingredients’ lowest level of concentration (LCL). Guidance for manufacturers is provided by the EPA’s Product Performance Test Guidelines; OCSPP 810 series that details the test methods to be used by disinfectant manufacturers to support claims of microbiocidal activity.4
In a similar manner to the BPR, the EPA recommends specific tests using specific reference microorganisms and product application techniques to substantiate disinfection claims. The Product Performance Test Guidelines include test methods from both the Association of Official Analytical Chemists (AOAC) and American Society for Testing and Materials (ASTM). The EPA has long preferred so-called “hard surface carrier” methods for substantiation of efficacy claims. Test surfaces called carriers are inoculated, dried, and then treated with the disinfectant. Most hard surface carrier methods are qualitative, meaning pass or fail determinations are made based on whether one or more test microorganisms survive treatment with a disinfectant. Some other methods are quantitative, meaning percent reductions are calculated by counting viable microbial populations before and after treatment with the disinfectant.
Good Manufacturing Practice
Pharmaceutical companies selling medicinal products in the EU are required to implement the necessary measures in order to comply with the requirements set out in EudraLex Volume 14 of the “Rules Governing Medicinal Products in the European Union — EU Guide to Good Manufacturing Practice.5 Pharmaceutical companies selling medicinal products in the United States are required to comply with the GMP requirements of Title 21 FDA CFR 211. Current Good Manufacturing Practice for Finished Pharmaceuticals.6 Part of these necessary measures include the design, validation and implementation of a documented and approved disinfectant programme. It will form a key part of any pharmaceutical production area qualification.
The current draft of Annex 1 of EU GMP 7, specifically covering sterile medicinal products has an expectation that cleaning and disinfection forms part of a facilities contamination control strategy. It states that the disinfection process should be validated. Validation studies should demonstrate the suitability and effectiveness of the disinfectants in the specific manner in which they are used and should support the in-use expiry of prepared solutions. The U.S. FDA Guidance for Industry, Sterile Drug Products Produced by Aseptic Processing (Aseptic Processing Guide September 2004) 8 states that each manufacturer must have a formal programme governing the qualification, use and disposal of disinfectants. The suitability, efficacy, and limitations of disinfecting agents and procedures should be assessed. The effectiveness of these disinfectants and procedures should be measured by their ability to ensure that potential contaminants are adequately removed from surfaces.
However, neither EU GMP nor US FDA guidance make any specific reference to disinfectant efficacy test standards. Neither mention the pass criteria that need to be achieved for an individual disinfectant, the decision on level of microbial kill will be based on room grade, environmental monitoring, risk assessment and form part of the contamination control strategy for the facility. However, both mention the importance of the pharmaceutical manufacturer evaluating the efficacy of disinfectants used both, in the manner in which they are to be used and on the surfaces they will be used. Regulators in both Europe and NA will expect to see disinfectant qualification and validation.
Even though a cleanroom disinfectant needs to be authorised / approved with the relevant biocidal registration system, the GMP regulations do not specify that this has to be the case. However, using an authorised disinfectant gives reassurance of continuity of supply (an unauthorised disinfectant could be pulled from the market) and independent health and safety and efficacy information.
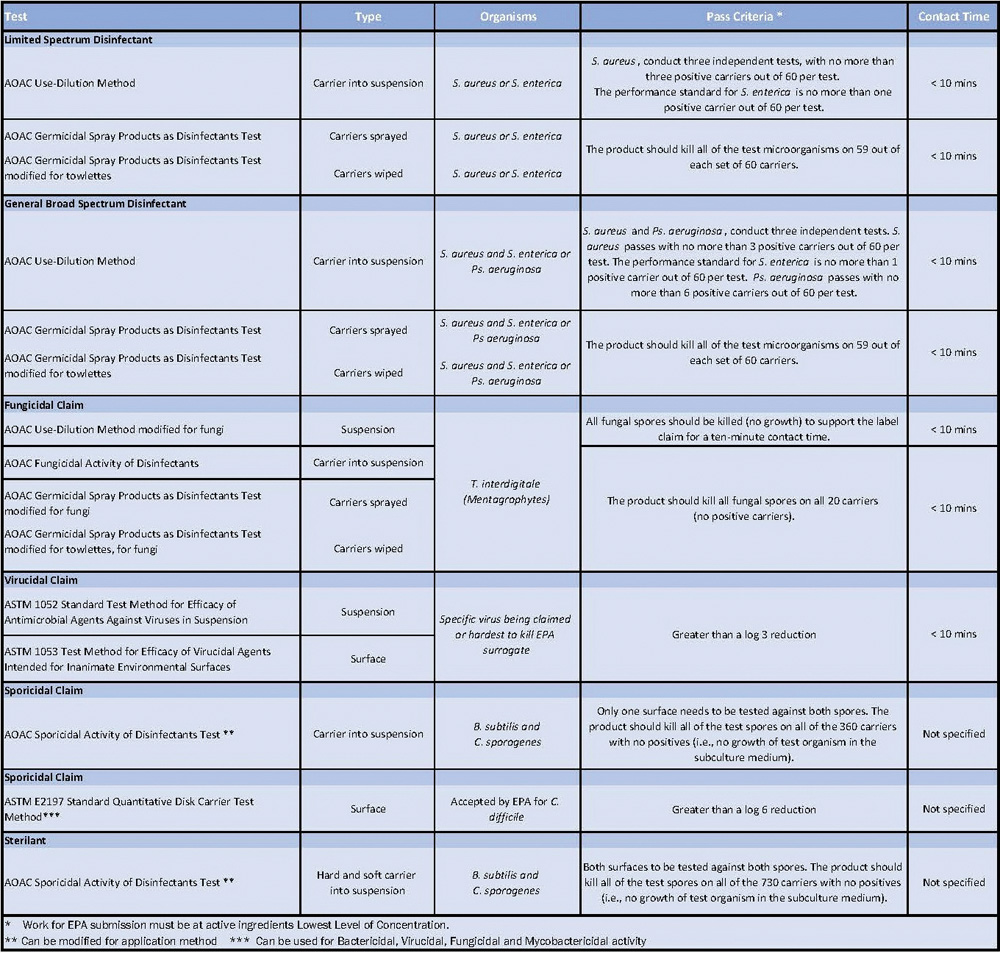
US test methods useful for testing disinfectants in cleanrooms.© Contec
European Efficacy Tests
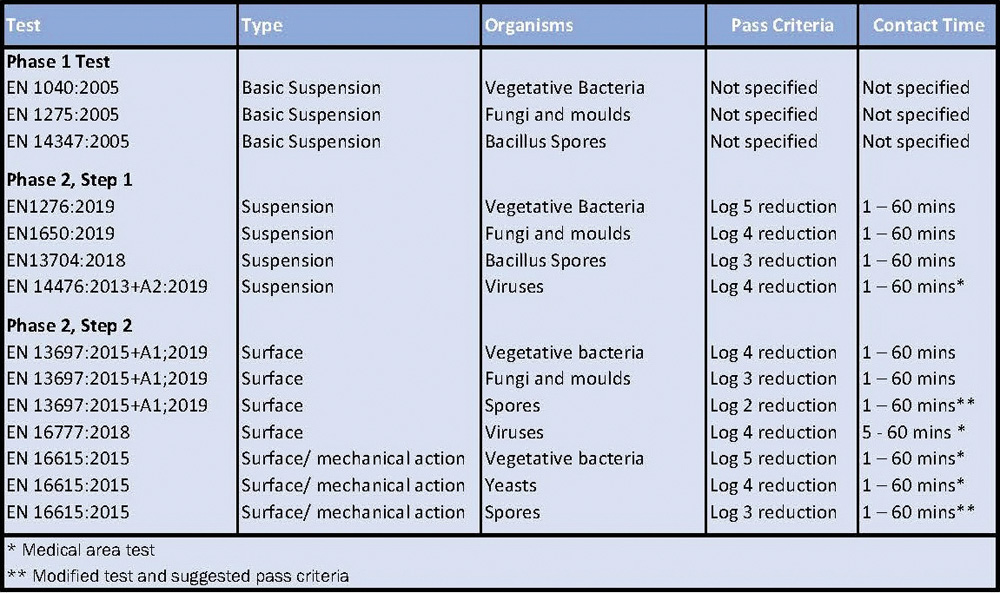
A facility which needs to validate a disinfectant in Europe has a structured series of tests devised by the CEN Technical Committee (TC/216) to use. This structure is highly accepted by member state GMP regulators.
The CEN disinfectant test methods are summarised in EN 14885:2018 9, a very helpful “Standard of standards” which specifies the European Standards to which products have to conform to claim microbial activity. It covers methods for vegetative bacteria, fungal spores, yeasts, viruses, mycobacteria and bacterial spores and is applicable to products to be used in the area of human medicine, veterinary areas, and in food, industrial, domestic and institutional areas. It is currently under revision as pr EN 14885:2020 (E).10
- Phase 1: Quantitative suspension tests to establish that a product under development has bacterial, fungicidal, yeasticidal or sporicidal activity without regard to specific areas of application.
- Phase 2:
Step 1: Quantitative suspension tests to establish that a product has bacterial, fungicidal, yeasticidal, mycobactericidal, tuberculocidal, sporicidal, virucidal, activity under simulated practical conditions appropriate to its intended use. These tests prove the irreversible inactivation of microorganisms but the activity of the product is against microorganisms in suspension.
Step 2: Quantitative non porous surface tests to establish that a product has bactericidal, fungicidal, yeasticidal, mycobactericidal, tuberculocidal, sporicidal, virucidal, activity when applied to a surface under simulated practical conditions. Phase 2, step 2 tests provide information against desiccated microorganisms on inanimate surfaces.
- Phase 3: Field tests under practical conditions.
The applicable methodologies for this type of test are not yet available, but may be developed in the future. Guidance on the design of phase 3 tests and the use of data from phase 3 tests is now provided in Annex C of EN 14885.
Tests must be carried out under the minimum/ obligatory conditions if specified in the standard. Additional test organisms, temperature, contact times and interfering substances can also be carried out but must be specified. Generally both Phase 2, step 1 and Phase 2, step 2 tests are needed in combination to support efficacy claims.
Currently, there is not a Phase 2, step 2 test for testing disinfectants with mechanical action in industrial areas (one is currently in progress), but there is one available for the medical area so this is used. Medical area tests are also used for virucidal testing. There is provision to use a standard from another area if one doesn’t exist, modifications can also be made but the modification has to be declared and state the product was tested in accordance with the principles of “X“ EN test.
The standards are routinely updated or amended and this can be seen by the date following the standard number, Eg EN 13697:2015+A1;2019.11 The foreword of the standard will state if any changes have been made which might impact the results from a previous version: “The changes mentioned above have no impact on the test results obtained with reference to the previous version. Those results are still valid.” Or, “The changes mentioned above have an impact on the test results obtained with reference to the previous version. Products have to conform to this new version in order to support the claims for the activity corresponding to this European Standard”. Be aware when looking through manufacturers data as very often results will just be declared to a particular test without the standard’s date being specified. This was especially relevant when “spiny spores” were added to EN 1650 12 and EN 13697 11 test methods. Disinfectants which had passed the previous tests, would not always pass the new test method. 70 % IPA solutions are an example of this.
United States Efficacy tests
While any antimicrobial product could be validated, most facilities use products that are already EPA registered as disinfectants. The pass/fail criteria for cGMP disinfectant validations are considerably different than for EPA registration as a disinfectant. A facility may chose to validate with a more dilute version of a concentrate or a shorter contact time. The procedures used for validation should be scientifically sound and are often based on existing standards, but with opportunities for modification (e.g., lower inoculum, no soiling).
EPA registration requirements do not address how disinfectants are used in pharmaceutical, biotechnological, and medical device industries. Manufacturers within these industries are instructed to validate disinfectants by demonstrating efficacy through the following analyses:
- Use-Dilution tests against a wide range of standard organisms and environmental isolates specific to a particular location.
- Surface challenge tests using standard organisms and typical environmental isolates specific to a particular location, applying disinfectants to surfaces at the specified concentration and contact time.
- Statistical comparisons of the frequency of isolation and number of microorganisms isolated before and after implementing a new disinfectant or protocol.
It is worth bearing in mind especially when reviewing the literature from a US disinfectant manufacturer that the definitions for sanitizer, disinfectant and sporicide differ in the US to those commonly used in Europe. The EPA defines a sterilant as something used to eliminate or destroy: fungi, fungal spores, viruses, vegetative bacteria, bacterial spores and can be a liquid chemical sterilant used by immersion. A steriliant is used to inactive spores on both hard and soft inanimate surfaces. The product should kill all of the test spores on all of the 720 carriers with no positives against (AOAC) Official Method 966.04 Sporicidal Activity of Disinfectants test. A sporicide is used to inactivate bacterial spores on a single chosen inanimate surface, the product should kill all of the test spores on all of the 360 carriers with no positives against (AOAC) Official Method 966.04 Sporicidal Activity of Disinfectants test.
Disinfectants are defined as something used on nonliving surfaces and objects to destroy or irreversibly inactivate infectious fungi and bacteria but not necessarily their spores. A broad spectrum disinfectant has a label claim against both Gram-negative and Gram-positive bacteria, a limited specturm disinfectant has activity against one but not both. A sanitizer is defined as a product which is used to reduce but not necessarily eliminate microorganisms from the inanimate environment to levels consider safe by public health codes or regulations.
The validation of disinfectants in cGMP environments in the US is conducted with a variety of official and non-official methods using guidelines from for example USP <1072> 13, PDA TR#70 14 and other documents. USP <1072> goes on to state that disinfectant efficacy studies must have realistic acceptance criteria, at least 2-log reductions for bacterial spores and 3-log reductions for vegetative bacteria. The Table shows commonly used AOAC and ASTM disinfectant efficacy test methods.
In summary, it is very clear from the GMP regulations that pharmaceutical manufacturers need to design, validate and implement, a documented and approved disinfectant programme as part of their contamination control strategy. There are many standard disinfectant efficacy test methods available in both Europe and the United States but the testing approach is very different and using the tests in the opposing regions is not so easily accepted. Currently there are very few, maybe only two disinfectants, which are approved for use in both North America and Europe, available with a data package of both EN and AOAC/ASTM testing. Guidance documents are available to help create the disinfectant validation plans for an aseptic facility and disinfectant manufacturers and test labs will help with the design and implementation of a disinfectant efficacy testing programme.
Author: Karen Rossington, Contec Inc.
References
1 EU Biocidal Product Regulation 528/2012
2 Title 40 of the Code of Federal Regulations (40 CFR) Subchapter E Pesticide Programs Parts 150-189
3 ECHA Guidance on the Biocidal Products Regulation Volume II Efficacy - Assessment and Evaluation (Parts B+C) Version 3.0 April 2018
4 EPA Product Performance Test Guideline, OCSPP 810.2100, Sterilants, Sporicides, and Decontaminants, Guidance for Efficacy Testing,
4 4 EPA Product Performance Test Guideline, OCSPP 810.2100, Sterilants, Sporicides and Decontaminants, Guidance for Efficacy Testing and OCSPP 810.2200, Disinfectants for use on Environmental Surfaces, Guidance for Efficacy Testing
5 EudraLex Volume 4 EU Guidelines to Good Manufacturing Practice Medicinal Products for Human and Veterinary Use
6 The Code of Federal Regulations CFR Title 21 - Food and Drugs: Parts 1 to 1499
7 Annex 1 Manufacture of Sterile Medicinal Products (Draft v.12, issued February 2020)
8 FDA Guidance for Industry - Sterile Drug Products Produced by Aseptic Processing, Current Good Manufacturing Practice (2004)
9 EN 14885:2018 Chemical disinfectants and antiseptics – Application of European Standards for chemical disinfectants and antiseptics.
10 Pr EN 14885:2020 (E) Chemical disinfectants and antiseptics – Application of European Standards for chemical disinfectants and antiseptics. (draft for comment)
11 EN 13697:2015+A1;2019 Quantitative non-porous surface test for the evaluation of bactericidal and/or fungicidal activity of disinfectants used in food, industrial, domestic and institutional areas. Test method and requirements (phase 2, step 2)
12 EN1650:2019 Chemical disinfectants and antiseptics –Quantitative suspension test for the evaluation of fungicidal or yeasticidal activity of chemical disinfectants and antiseptics used in food, industrial, domestic and institutional areas – Test method and requirements (phase 2, step 1)
13 United States Pharmacopoeia (USP) General Chapter <1072> Disinfectants and Antiseptics
14 Parenteral Drug Association (PDA) Technical Report No. 70. The Fundamentals of Cleaning and Disinfection Programs for Aseptic Manufacturing Facilities (2015).
CEN = European Committee for Standardization
OECD = Organisation for Economic Co-operation and Development
ISO = International Organization for Standardization
AOAC = now AOAC International
ASTM = now ASTM International
VAH = Verbund für Angewandte Hygiene e.V.
AFNOR = Association Française de Normalisation